DVT (Deep Venous Thrombosis)
Definition of DVT (Deep Venous Thrombobis)
DVT, or Deep Venous Thrombosis , is the formation of blood clots (also known as thrombus) within the deep veins of the body. The most common locations are the legs, followed by the pelvis. DVT is a relatively common medical condition, affecting up to 600,000 Americans each year. Over 1 million people undergo evaluation for DVT annually in the United States.
 Symptoms of DVT
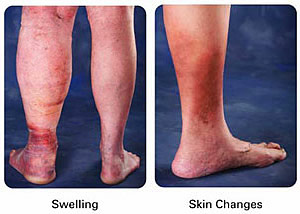
Symptoms of DVT
At least 50% of those with deep venous thrombosis have no symptoms at all and the condition is discovered by imaging studies alone. Symptoms of DVT include pain, swelling (also known as edema), skin discoloration (red, pink, purple, blue, or tan), tenderness of the leg, enlarged or engorged veins, increased warmth of the skin, and “tightening” of the skin.
Cause of DVT
The etiologies of deep venous thrombosis are multiple. They include prolonged immobilization (such as during prolonged travel), surgery, physical trauma, pregnancy, medications such as hormone therapy and birth control medications, obesity, cancer, genetic or inherited clotting disorders, vein catheters, May-Thurner’s Syndrome, advanced age, and infections.
Some known predisposing factors that lead to the veins clots forming include decreased blood flow within the veins (i.e. venous stasis), damage to the blood vessel walls and the valves located within the vein walls, and thickening of the blood itself (known as hypercoagulability).
Diagnosis of DVT
The most common way that deep venous thrombosis is diagnosed is through a vein ultrasound, also known as a venous duplex study. Other methods of diagnosis include CT scan (CAT scan), MRI, and catheter venography. Physical exam by a doctor can aid in the diagnosis, but a confirmatory imaging test is always necessary.
 Complications of DVT
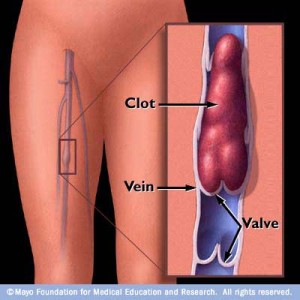
Complications of DVT
The most dangerous complication related to deep venous thrombosis is the clot spreading or traveling to another location of the body. If the clot dislodges and floats to the heart and lungs, it can lead to a Pulmonary Embolism (PE) than can be lethal.
Post-thrombotic Syndrome (PTS) is a chronic condition in which the veins become damaged long-term as a result of scar tissue formation or valve damage within the lining of the veins. This can lead to areas of obstruction or stenosis that hinders the ability of blood to circulate normally. If the valves are dysfunctional within the veins, this can lead to venous insufficiency or venous reflux, a chronic circulatory disease. This often is referred to as “venous hypertension” of the leg. The symptoms of this condition include long-term leg swelling / edema, chronic leg pain that is often worse with walking or prolonged standing, skin damage that often manifests as brown discoloration at the ankles, or skin ulcers of the leg (most often located on the inside of the ankles).
Treatment of DVT
There are many different treatment options available for deep venous thrombosis. The type of treatment offered by your physician often depends on the location and severity of the clots. The most common treatment offered is anticoagulant medications, either Coumadin (Warfarin), Lovenox, Heparin, or a combination of these. When these medications cannot be administered for medical reasons (such as risk of bleeding), a metal filter device is often placed within the vein (known as an Inferior Vena Cava Filter or IVC filter). IVC filters can often be removed at a future date when they are no longer needed. Other common therapies include “clot-busting” or “clot-dissolving” medications that can be delivered through a catheter directly into the clot under x-ray guidance. One such medicine is referred to as t-PA or Tissue Plasminogen Activator. Other possible therapies for regions of vein obstruction or stenosis that do not respond to the medications include balloon angioplasty or stents placed into the vein under x-ray guidance. It is best to have a consultation with a Vein Specialist as quickly as possible after being diagnosed with a DVT so that all of your options can be discussed.
Prevention of DVT
Deep venous thrombosis preventative measures to are advised for at risk medical, surgical, and pregnant patients. Prophylaxis includes early and frequent exercise / movement, compression stockings, pneumatic compression devices, and blood-thinner medications such as heparin and Lovenox. Please consult with a physician to find out which options are best for your particular situation.








