Varicose & Spider Veins | Definitions & Vein Treatment

What are Veins?
Veins are blood vessels that return blood to the heart once it has circulated through the body (as opposed to arteries, which carry oxygen-rich blood from the heart to the body). Healthy veins carry the non-oxygenated blood back to the heart and lungs so that the blood cells can be replenished with oxygen, allowing the refreshed blood to be reenter the circulation once again. Veins have one-way valves that help keep blood flowing in the proper direction (i.e. toward the heart).
VARICOSE VEINS
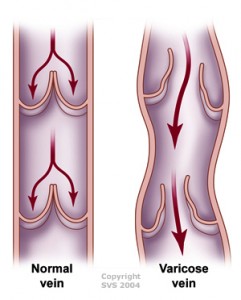
If these vein valves stop functioning in the way that they are supposed to, blood begins to flow backwards and pool in the veins, raising the blood pressure in the veins themselves. This process leads to a vein disease called venous hypertension and venous reflux disease.
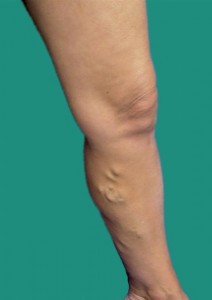
The build-up of pressure within the diseased veins leads to the vein walls stretching and thinning. This process leads to the development of unsightly enlarged and bulging veins beneath the surface of the skin. These abnormal stretched and enlarged veins are known as varicose veins.
Varicose veins are swollen, dark blue or purple blood vessels that you can obviously see and feel beneath the skin. They often look like twisted cords, and usually appear on the calves, inside of the legs, and ankles. As varicose veins continue to weaken under the constant strain, they often continue to get bigger and balloon outward. This tends to raise the skin surface and causing the skin to bulge and thin out or get discolored.
Patients with varicose veins often develop aching, throbbing, cramping, burning, itching and other symptoms that may indicate a need for medical attention. Other patients with varicose vein disease may remain without symptoms for years.
Varicose veins are considered a “disease” since the valves within the veins are defective and the blood flow within these veins is backwards. The disease process does tend to spread to other areas of the legs over time, as the leg veins are connected to one another through a series of branch connections. These vein connections allow the venous hypertension to spread from diseased varicose veins to healthy vein segments. It is often described as a “domino effect” of more and more vein valves breaking as they are exposed to the elevated vein pressure from adjacent diseased veins. Therefore, varicose vein disease does tend to worsen over time and begins to involve larger and larger areas of the leg. The sooner the condition is treated, the easier it is to deal with medically.
Risks Factors For Varicose Veins
While varicose veins can affect nearly anyone of any age, they tend to occur more often in patients possessing certain risk factors, including:
- Older age
- Family history of varicose veins
- Pregnancy, especially multiple pregnancies
- Obesity
- Lack of physical activity
- Excessive sun exposure
Although the risk tends to increase with age, varcicose vein are often seen at very young ages, even in the teenage years.
Diagnosing Varicose Veins
Your doctor can usually diagnose varicose veins and any associated venous conditions after a physical examination of the affected area. Additional testing may also be required, such as a venous ultrasound or venous reflux study. These studies allow the physician to obtain an anatomical “road map” of your circulation. This allows for more precise and targeted treatment options.
When to Consider Vein Treatment
If varicose veins are leading to any symptoms, one should consider medical evaluation of your venous disease. Patients report a wide variety of symptoms including burning or aching pain, throbbing, itching, and pressure sensations. Leg or ankle swelling is also a prominent complaint in those with varicose vein disease. Both discomfort and swelling can be signs of significant underlying circulation issues such as venous reflux which requires additional testing for diagnosis.
While many of those suffering with varicose veins may not have leg discomfort, many patients with varicose veins are bothered by their appearance. Cosmetic reasons alone are the most common reason patients seek vein treatment for varicose veins and spider veins.
Patients often report embarrassment and reluctance to wear shorts or skirts. The condition can lead to avoidance of social activities or sports or the eroding of one’s self-confidence. They can even be the root of psychological problems related to body perception such as body dysmorphic disorder.
Long-standing varicose vein disease can lead to many different problems, some more serious than others. The problems that can arise over time include chronic wounds or ulcers in the feet and ankles (e.g. venous stasis ulcers), chronic leg or foot swelling or edema, discoloration or darkening pigment changes in the skin, thinning of the skin or other severe skin disorders including stasis dermatitis, recurrent thrombophlebitis, and increased risk of skin infections such as cellulitis. The longer that the varicose vein disease is present, the higher the likelihood of developing these more complicated medical issues.
Pain or discomfort symptoms in the legs can also be the signs of more serious underlying medical conditions in the veins as well. Both phlebitis / thrombophlebitis as well as deep venous thrombosis can lead to pain or swelling in the veins of the leg. These conditions are best diagnosed by physician through a physical exam and vein ultrasound study.
Treatment of Varicose Veins
There are many reasons people seek treatment for varicose veins, including frequent discomfort, chronic swelling / edema, or skin damage. Many people with venous disease also seek cosmetic vein treatments to eliminate or reduce the appearance of unsightly varicose or spider veins on their legs. Sometimes patients seek out vein treatment to reduce their chances of developing more significant circulation problems down the road if their veins are left untreated.
There are several treatment options available to eliminate or reduce the appearance of veins and relieve any symptom. These therapies may include self-care methods such as losing weight, keeping the legs elevated, using over-the-counter anti-inflammatory medications, regular exercise, and wearing compression stockings.
More immediate and permanent relief is often achieved through interventional vein therapies. With advancements in technology, vein treatments can be administered with minimal discomfort and very fast recovery. Some of the more common and effective therapies include sclerotherapy and laser therapy.
- Sclerotherapy treats varicose veins by injecting a solution into the targeted veins that causes them to gradually disappear. The sclerosant solution used during the procedure irritates the vein lining and turns it into scar tissue that eventually fades away. Depending on the extent of your disease, it may require several vein treatment sessions to achieve the desired result.
- Endovenous laser therapy (EVLT) is a minimally invasive laser procedure that treats varicose veins faster, safer and more effectively than surgical procedures, as it precisely targets the affected veins with a laser probe under ultrasound guidance. The laser energy delivered to the vein causes the vein walls to scar shut so that blood can no longer flow through them, causing the varicose veins to shrink and fade. Following laser vein treatment, the venous blood flow that once circulated through the varicose veins is diverted into healthy veins.
- Radiofrequency vein ablation, which also goes by the Venefit VNUS closure procedure, is a office-based varicose vein treatment that utilizes oscillating radiofrequency waves to create a focused heat energy to close and ablate varicose veins. This vein treatment is associated with very little discomfort and has an 98% effective rate on treating varicose vein conditions.
For more information regarding treatment options, please refer to the other pages of our website.
Preventing Varicose Veins
While there is no surefire way to prevent varicose veins from developing, there are certainly life changes that can be made in order to reduce your risk of developing further problems with this condition. This may include:
- Exercising regularly
- Maintaining a healthy weight
- Eating a diet high in fiber and low in salt
- Elevating the legs
- Avoiding sitting or standing in one position for too long
Your doctor will provide you with more information as to how you can reduce your risk of varicose veins and maintain strong vascular health. There are various home remedies for varicose veins that can be very useful in reducing symptoms and risks.
SPIDER VEINS
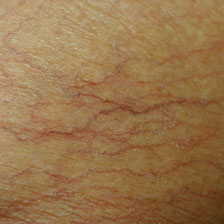
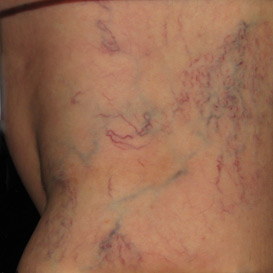
Spider veins, also known as telangiectasias, are small, thin blood vessel clusters that are easily visible within the skin. They are often red, pink, or purple and are usually dispersed as clusters in certain locations of the body. They appear most commonly on the legs, but may be seen anywhere on the body, including the face. They typically have the appearance of a series of lines, tree branches or a spider- web-like shape (hence the name). They tend to be much smaller than varicose veins, somewhere in the range of size of a small thread or at most a toothpick. It is very common for people to seek out cosmetic therapies to rid their skin of these unsightly veins. While most cases of spider veins are of purely cosmetic concern, some patients may also experience uncomfortable symptoms such as aching, burning, swelling, itching, and cramping from this condition.
Many patients are bothered by the appearance of spider veins on prominent areas of their bodies such as the legs or face, and seek treatment to restore a smooth, clear appearance. Many of these treatments are highly effective and minimally invasive, offering aesthetically-pleasing results without painful or lengthy downtimes.
Causes of Spider Veins
Spider veins develop as a result of a backup of blood in certain veins, which may occur when the valves in the veins cannot effectively keep blood from flowing backwards as it moves up the legs. As blood collects in the vein, it begins to expand and becomes visible under the surface of the skin or within the skin itself.
Spider veins are common in the legs because of the fact that blood flow must work against gravity to travel back up to the heart, with the legs having to carry the largest burden of gravitary blood flow. This condition affects nearly half of all adults over the age of 50 in the US, and may occur as a result of hormonal changes, pregnancy, obesity, trauma, sun exposure and genetic predisposition. You are much more likely to develop spider veins is you have immediate relatives with the same condition.
Your doctor can diagnose spider veins through a physical examination and will determine an appropriate treatment method based on a thorough evaluation of your condition and medical history. An ultrasound may be performed to evaluate the severity of the condition and identify the underlying cause to ensure the most effective treatment approach.
Treatment of Spider Veins
There are several minimally-invasive aesthetic treatment options available to eliminate the appearance of spider veins and allow patients to once again proudly show off their legs. Newer vein treatment options offer patients few side effects, less pain and shorter recovery times than traditional vein removal procedures.
One of the common and standard treatments for spider veins is sclerotherapy. Sclerortherpy involves injecting a sclerosing solution directly into the affected veins, causing them to gradually disappear. This procedure is typically performed in the doctor’s office and takes less than an hour. Depending on the extent of their vein disease, patients may require one to four treatment sessions in order to achieve their desired result. Additional vein treatment options for spider veins may include surface laser therapy, in which thermal energy delivered to the skin is used to eliminate the veins.
Mild cases of spider veins may also be treated with compression stockings to put pressure on the veins and promote normal blood flow. Your doctor will discuss with you what he feels are the best options for treating your condition based on your desires and expectations.
Prevention of Spider Veins
While there is no sure way to prevent spider veins from developing, there are certainly life modifications that can help reduce the risk of developing this unsightly condition. These include losing weight, exercising regularly, wearing support hose and wearing comfortable, supportive shoes. It is important to move the legs frequently, especially if your job requires long periods of sitting or standing in one place. Your doctor will provide you with specific guidelines to effectively reduce the risk of spider veins so that you can maintain beautiful and youthful appearing legs for many years.
To learn more about spider veins and the minimally- invasive treatments options available, please call us today to schedule an appointment. Or visit our Contact Page to request an appointment by email.